2020 was an extraordinarily difficult year [President's message]
2020 was an extraordinarily difficult year for the community and the medical profession. We dealt with threats to our personal health and the health of our families, threats to our livelihoods, and incredible disruption in almost every aspect of our lives.
Victorian doctors in particular have borne the brunt of the pandemic in Australia and understand better than most of us the terrible situation in many other parts of the world. I have been very proud of the response of the medical profession in these difficult times and it has been a great privilege to represent our profession on the national stage.
I would like to take this opportunity to update you on AMA activities over the last six months, and my priorities for the year ahead.
Some of our advocacy you will have seen in the media but there is a huge amount of behind-the-scenes activity that you may not be aware of. Despite an inability to travel and meet face-to-face, the AMA has been working hard on behalf of the medical profession. These are a few of the highlights.
- COVID-19
- Private specialist practice
- General practice
- Doctors in training
- Rural doctors
- Medical regulation practice
- Aged care
- Public health
- The year ahead
COVID-19
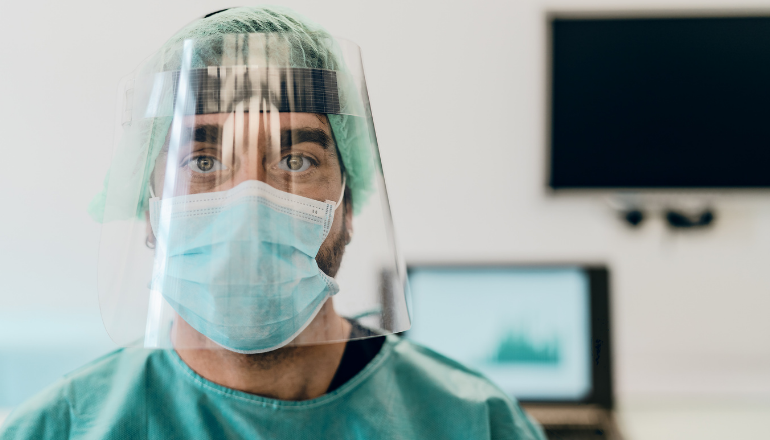
Any discussion of 2020 must start with COVID-19. The AMA led the profession in advocating early and hard for appropriate actions to control the spread of the virus, supporting our State and Federal Governments as they brought in restrictions and border controls, with the safety of frontline healthcare workers who put their lives at risk at the forefront of our actions at all times. These activities remain works in progress, and COVID-19 will continue to dominate our public advocacy in 2021.
AMA Federal Council COVID Communique
The Federal Council COVID-19 Communique in September was a call to action to all levels of government to ensure that the sacrifices made over the past six months of restrictions and lockdowns, family separations and financial setbacks were not squandered.
In particular, we reinforced the need for ongoing vigilance and social distancing to minimise the risk of lockdowns in the inevitable event of further outbreaks, due to breaches of quarantine. We have been calling for national consistency in the response to outbreaks and, whilst there has been some progress, this goal remains elusive.
Our predictions were sadly proven correct, with outbreaks in South Australia, New South Wales, Victoria and Queensland, and very different responses from the various State governments.
We only need to look at the horrific situations in the US, UK and Europe to see the results of a relaxed attitude to COVID-19. The best way to protect our economy, our jobs and our health care system is to protect our community from this virus.
PPE
Doctors and other healthcare workers were devastated by the lack of action by State and Federal governments to properly protect them from COVID-19. Thousands of doctors, nurses, and aged care workers in Victoria contracted COVID-19, demonstrating the failure of PPE guidelines and workplace safety regimes to protect frontline staff. The Infection Control Expert Group (ICEG) failed to recognise the potential for aerosol spread of the virus in health care settings and was reluctant to update national guidelines according to the precautionary principle.
The AMA relentlessly called out these failures. We successfully argued for the Senate Committee inquiry into COVID-19 to be reopened, to examine the impacts of COVID-19 on the healthcare workforce. Next week, I will be appearing before the reconvened inquiry to put forward the views and experiences of AMA members throughout this pandemic.
In September, the Government established a new National COVID-19 Evidence Taskforce, national surveillance of healthcare worker COVID-19 infections, and a new national network of epidemiologists. Minister Hunt and I released a joint statement, which can be read here.
The Taskforce’s job is to review the evidence and expert opinion from workplace safety experts, occupational hygienists and front-line healthcare workers in order to update the national guidelines. This process has been painfully slow to get going, but we are expecting an outcome early this year.
As AMA President, I am now a member of the Australian Commission on Safety and Quality in Health Care (ACSQHC) National Clinical Taskforce, representing the medical profession in ensuring that healthcare workers are protected from infection.
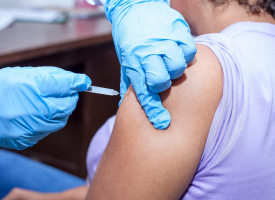
Vaccines
A successful vaccination program is the only way that we will be able to resume a relatively normal life any time soon. The challenge of developing, approving and distributing vaccines for the entire population of the world is extraordinary, particularly as there has never been a successful coronavirus vaccine in the past, but we are already seeing many countries start vaccination programs only a year after COVID-19 was first reported.
The AMA has been generally supportive of the Government’s approach to procuring vaccines but many challenges remain, and we will be working hard to ensure that the vaccination program succeeds. Ongoing issues include the choice of vaccine, the approval process, distribution, prioritisation and the critical logistic challenges around vaccinating 25 million people, twice, at defined intervals.
There has been much commentary in recent weeks over the efficacy of one vaccine over another, potential adverse effects, and whether Australia is moving too fast or dragging its feet. The AMA has been in constant discussions with the TGA, the Department of Health, and Health Minister Greg Hunt about supply chains, safety, efficacy, and the critical role of general practice in rolling out the vaccines to the wider population.
After extensive lobbying, the AMA has GPs on two Australian Technical Advisory Group on Immunisation (ATAGI) Working Groups that are looking at the COVID-19 vaccine. This ensures the AMA will have significant insight into vaccine development and input into the implementation of any vaccine rollout.
The recent decision to roll the Pfizer-BioNTech vaccine out to high priority individuals through hospital hubs is reasonable, given the logistical challenges of maintaining a cold chain at minus 70 degrees Celsius. The broader vaccine rollout to the rest of the population is likely to use a different vaccine and will be built around general practice.
Private Specialist Practice
Two issues have dominated the private specialist practice agenda over the past few months – private health insurance and the aggressive moves of some health funds towards managed care, and the ongoing Medicare Benefits Schedule (MBS) reviews.
Private Health Insurance (PHI)
The AMA released its ‘Prescription for Private Health Insurance’ in August. This has been well received by the industry and government, with broad acceptance that the underlying problem with PHI is not doctors’ fees or poor experiences with private care, but the number of young people who are abandoning the system. Rising premiums and poor wage growth have made health insurance a weak value proposition for young people. Our community-rated PHI system relies on a pool of healthy people to subsidise the care of those with more expensive health needs, and this whole structure is now at risk.
The AMA called for a range of responses from Government, including addressing the declining value of the PHI rebate, tweaking Lifetime Health Cover loadings, increasing the Medicare Levy Surcharge and promoting discounts for younger members, as well as allowing young people to stay under their parents’ insurance cover for longer. This advocacy has been successful. Federal Government has agreed to extend the age at which young people can be covered by their parents’ policy from 25 years to 31. And as a result of our paper, the Government has also announced in the recent Budget a detailed actuarial study into some of the above current policy settings, with a view to reform.
Some insurers have been making direct moves to reduce the cost of claims in order to reduce the pressure on their premiums. We have seen direct contracting of doctors with insurers and hospitals to deliver short stay care or to reduce the use of inpatient rehabilitation. We have also seen Medibank Private purchase 49 per cent of the East Sydney Private Hospital, the site of one of these short stay models. This vertical integration is viewed very suspiciously by most of our industry and the confidential arrangements between doctors and insurers risk heading down a pathway to US-style managed care.
The AMA has met with medical groups, private hospitals, multiple insurers and government to discuss these issues over the past few months. We have committed to a sustainable future for private medicine in Australia and recognise that may mean change that affects our members. However, we cannot allow the insurers to determine the future of patient care in this country and we are taking direct action to resist changes already proposed by the insurance industry.
One example of this is the Prosthesis List, a construct unique to Australia that ensures choice of prosthesis for doctors and patients and determines the price paid by insurers for prostheses. This list is in need of reform in order to ensure that Australians are getting value for money for prostheses. However, plans to abandon it and potentially pass control to either hospitals or insurers were well advanced, prior to any input from doctors. This underlines the critical need for AMA to be engaged in this advocacy.
We believe that Government-led reform of PHI is far more likely to result in a sustainable industry than insurer-led cost-cutting and contracts, but there is also work for us as a profession to ensure that we are delivering value-based care in the interests of our patients and the long-term sustainability of private health care in Australia. It is heartening that 28 groups have now signed up to the AMA’s Informed Financial Consent Guide since its release in 2019.
MBS Review
Whilst most of the detailed input on the MBS reviews came from within individual specialties, the AMA has maintained a high-level view of proposed changes. As more of the MBS Review moves towards implementation, we need to remain vigilant and ensure that there is adequate clinical input into all aspects of the implementation plans.
We have been critical of the lack of transparency of many parts of the review process, including the Implementation Liaison Groups (ILGs) (which themselves were created as a result of AMA advocacy), but the most pressing issue now is the lack of notice once changes to MBS items are confirmed by the Parliament. In the case of the recent spine surgery changes at the beginning of the review, there was almost no notice provided to the AMA, insurers, software providers and workers’ compensation authorities. This resulted in procedures occurring without recommended or gazetted fees having been set, and very significant inconvenience and disruption for patients, insurers, hospitals and doctors.
Upcoming changes are far more significant than the spinal numbers and AMA has made it very clear to the Health Department that six months’ notice is required to enable smooth implementation. This is one area where collaboration with the hospital and insurance sector is important. A lack of notice impacts all three key players in the private system and hurts patients.
The MBS Review Taskforce has concluded its work, but there are several proposed changes that have been left in limbo. The AMA is seeking clarity on the status of these proposals to ensure adequate consultation before any attempt at implementation. Some of these proposed changes have been very controversial, such as timed specialist consultations and removal of surgical assistance item numbers.
General Practice

Telehealth
The COVID-19 pandemic has had a very significant impact on general practice and this was recognised early by the Government. After years of AMA advocacy, Medicare-funded telehealth item numbers were made available on a temporary basis and gradually tweaked to make them more fit-for-purpose.
I was very pleased to join Minister Hunt when he announced that telehealth item numbers would become permanent. We are still working with Government and other stakeholders, including the RACGP, on the detailed planning. It is expected that access to GP telehealth will be linked to voluntary patient enrolment and we are working to ensure that rebates for telephone consults are at the same level as video consults at least during an implementation phase.
Workforce distribution training
The AMA continues to represent the profession in discussions with government around GP workforce planning and distribution. We have led calls for changes to the model of employment for GP registrars to make GP training more attractive to junior doctors. We have engaged in discussions with all stakeholders and recently held a planning session with many of those stakeholders.
Similarly, the AMA has been keeping a close eye on the upcoming changes to GP training, including the transition of training back to the Colleges. The Government wants to maintain levers to control workforce distribution, but it is critical that the Colleges maintain enough control of selection, training and standard setting to be able to guarantee the quality of the GP workforce going forward.
The AMA released its updated Vision Statement for GP Training in December, calling for consideration of a single employer model and other measures to ensure general practice continues to be a desirable career option. The Department has agreed to include the AMA on a key advisory group to provide direction on potential GP training reforms.
Primary care reform
The AMA‘s Delivering Better Care for Patients: The AMA 10-Year Framework for Primary Care Reform highlights the central role of general practice in health care. It identifies immediate funding goals to ease the financial pressures on GPs, and long-term reforms that must be implemented as part of the Federal Government’s 10-year Primary Health Care Plan.
We have successfully advocated for reforms to remove the requirement for GP CPD to be reported via the GP Colleges, and to allow GPs to access to A1 rebates directly linked to their specialty recognition with the Medical Board of Australia.
The Government has maintained its commitment to a voluntary patient registration scheme, which will underpin blended funding mechanisms to better support general practices in delivery of value-based, longitudinal and comprehensive care.
I’m pleased that we’ve also seen improvements to incentives to support doctors working in rural areas and general practices, but clearly there is much more work to do. Ensuring the general practice workforce into the future is a high priority for us and we are exploring how our GPs in Training can be supported through potential reform in their employment arrangements.
Doctors in Training
Our AMA Council of Doctors in Training (CDT), led by Dr Hash Abdeen, has continued its excellent work advocating for the welfare and training of our junior doctor workforce. I was pleased to join representatives of Everymind, Australian Medical Students’ Association, and other groups at the launch of ‘Every Doctor Every Setting National Framework in October.
But we were also acutely aware of the other challenges facing our Doctors in Training. To that end, the AMA has also met with the RACGP and ACRRM to discuss their exam failures, and how to best support trainees through the trauma of the abandoned exams.
The Specialist Traineee Experience Health Check – a report card on how the various Colleges are delivering training – was also released in November, furthering our focus on these important issues.
And the AMA will soon be releasing Position Statements on Prevocational Medical Education and Training, and Medical Parents in Training. I’d like to thank all our Doctors in Training for their contributions to this work.
Rural Doctors

The AMA Council of Rural Doctors (CRD), under Dr Marco Giuseppin, has continued to raise concerns with the Government about barriers to private sector relocation to regional Australia, and the future of regional training organisations.
CRD is actively working with other key stakeholders to develop infrastructure to support more rural training for GP and non-GP specialists, and has provided extensive feedback on the review of the Rural Health Multidisciplinary Training Program.
The AMA is acutely aware of the need to keep COVID-19 out of our rural and remote communities, where local health services would be quickly overwhelmed, and this has been at the forefront of our advocacy to all levels of Government.
Medical regulation
The annual workshop of the AMA, the Medical Board of Australia (MBA) and the Australian Health Practitioner Regulation Agency (AHPRA) was held on 12 August 2020. The workshop is a key opportunity for the leadership of the AMA to raise member concerns, particularly those related to the handling of complaints by AHPRA and the MBA.
Following years of advocacy concerning the issue of vexatious complaints, AHPRA and the Medical Board released a vexatious complaints framework on 10 December 2020. The framework enables vexatious complaints to be identified and managed earlier in the notification process, thereby hopefully reducing harm to our profession.
CDT continues to work with the MBA to provide input on the design, administration, analysis and communication of the results of the Medical Training Survey (MTS) results.
Aged care
COVID-19 exposed the massive failings in our aged care system, and the AMA has continued to advocate for immediate action to reform the obvious flaws in the care of our most vulnerable citizens. This backed our detailed outline to Government of what the AMA felt was required in aged care to better prepare the aged care sector for COVID-19.
But we all know the aged care system, particularly with regard to health care in nursing homes, was broken long before COVID-19. The AMA has made numerous submissions to the Royal Commission and Dr Chris Moy, AMA Vice President and a GP with significant experience working with nursing homes, be talking to the Royal Commission again soon. In addition, I signed a joint letter with the Australian Nursing and Midwifery Federation calling for urgent action in aged care – an extension of our ‘Care Can’t Wait’ campaign. We also released the final two Aged Care Position Statements from our revised suite of Aged Care Position statements, covering Medical Care of Older Australians and Palliative Care.
Public health
Vaping
The AMA has continued to argue against liquid nicotine products being made freely available in Australia, given the lack of substantive evidence of their efficacy as quit smoking aids, and the risk that they normalise smoking.
The TGA has upheld the AMA’s position, cracking down on liquid nicotine imports and making the substance available only on prescription. While the AMA does not support vaping for any use, we support the TGA decision on the basis that it closes the loophole that allowed private imports of nicotine vaping products. In prosecuting our position we’ve made submissions to both the TGA and the Parliamentary Committee inquiry, and I appeared with a number of other medical experts in front of the committee.
Climate Change and natural disasters
The AMA signed a Memorandum of Understanding with Doctors for the Environment Australia on climate change and sustainability in the health sector, transitioning to renewable energy, and a national strategy for health and climate change.
Our proposal for GPs to be involved in local, State, and Federal disaster planning and responses was one of the recommendations of the final report of the Bushfire Royal Commission. More broadly, the health impacts of climate change is an issue that I know many members are passionate about it, and one that I will continue to pursue with policy makers.
Sugar and Obesity
The AMA held a member-only “Sugar-Blinded” webinar with Australian of the Year, Dr James Muecke, in November.
In the coming months I will be talking more about prevention, sugar and obesity in detail – including devoting some of our research capacity to the task of developing policy options for Government consideration. For too long prevention has remained underfunded and forgotten. I hope in my time as AMA President I am able to elevate it to become a key pillar of health policy.
Indigenous helath
In December, I was privileged to present the 2020 AMA Indigenous Medical Scholarship to Lloyd Diggins, a third-year University of Notre Dame Australia medical student who plans to work as a GP in remote communities. Lloyd’s acceptance speech was a blistering summation of the casual racism that still exists in our healthcare systems.
Nominations for the 2021 scholarship close on 31 January. I encourage you to share the details with your colleagues. A key step towards closing the gap is to grow the Aboriginal and Torres Strait Islander medical workforce.
The year ahead
Colleagues, 2020 taught us many things. Our public hospital system, already under-resourced and under strain, coped with the COVID crisis – just. This year, we will see many more challenges as the fallout from last year’s lockdowns and elective surgery cancellations catches up with us. This year’s Public Hospital Report Card will be even more important than ever.
Australia is very lucky that we have been able to keep COVID-19 out of our remote Indigenous communities, where its effects would be devastating. Our Aboriginal community-controlled health organisations have played an outstanding role in keeping these vulnerable communities safe, and we must support them to continue in these efforts.
COVID-19 has so far largely been an issue in our major urban areas. But we cannot afford to overlook our rural health networks in our advocacy for the best health outcomes for all Australians.
In coming weeks, you will be hearing much more from the AMA about public health, aged care, and the AMA’s strategy for the future. I promise to write again soon and keep you updated on how your AMA is working for you, your patients, and your community.
Yours Sincerely,
Dr Omar Khorshid
AMA President